Introduction: It is recognized that many people living with sickle cell disease (SCD) face significant structural obstacles to establishing and maintaining long-term hematology care. For example, some people with SCD care may lose access as a result of a geographic move; others may lose access by aging out of the pediatric care setting. These scenarios could be addressed by providing resources in areas with addressable populations and unmet medical need. However, deploying SCD treatment resources is frustrated by the lack of an established tool that can estimate the number of people living with SCD or gaps in services available in a given geography. We hypothesized that we could build a tool using a combination of publicly available demographic data combined with hospital claims data.
Methods: Using CDC estimations for SCD affecting 1 in 365 African American and 1 in 16,300 Hispanic births, we estimated SCD prevalence based on data from the 2021 US Census, segmented by age, race, and county. We added a distinction between rural and urban counties using classification from the Consumer Financial Protection Bureau (CFPB), which designates rural counties as “a county that is neither in a metropolitan statistical area nor in a micropolitan statistical area that is adjacent to a metropolitan statistical area.”. PowerBI was used to generate a heat map to visualize the data at a state and county level, with the ability to filter by patient age and urban vs. rural designation. Finally, using hospital claims data for SCD “with crisis” (i.e., claims referencing ICD10 codes: D5700; D5701; D5702; D57211; D57212; D57219; D57811; D57812; D57819) and SCD “without crisis” (i.e., claims referencing ICD10 codes: D571; D5720; D5740; D5742; D5744; D5780), Pearson correlation was used to determine if an association existed between our estimated SCD prevalence and SCD related hospital claims for claim years 2021, 2022 and partial 2023.
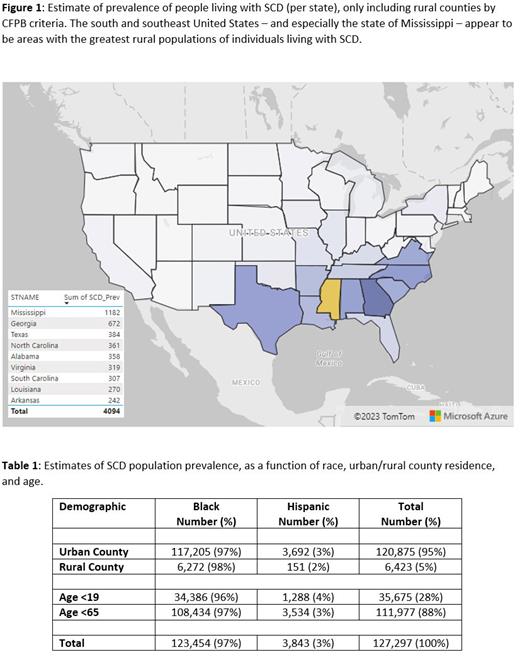
Results: Our model estimates a total of 127,297 people living with SCD in the United States, with 97% (123,454) being Black and 3% (3,843) being Hispanic (Table 1). 88% (111,977) were predicted to be under age 65, and 28% (35,675) were predicted to be under age 19. The majority (95%, 120,875) lived in urban counties. Most rural counties with SCD patients are located in the South and Southeast US (Figure 1). There was a strong positive correlation between our predictions of SCD prevalence at the state level and SCD-related hospital claims (coefficient of 0.903217 [95%CI: 0.944-0.836], p<0.001). For claim years 2021, 2022 and 2023 (partial) there were 1.6 claims per 1 SCD patient across the United States. While there were 1.6 claims per patient in urban counties, there were 0.7 claims per 1 patient in rural counties, consistent with a relative lack of access to care in rural areas compared to urban areas.
Conclusions: Although not a direct measurement, and possibly overestimating the number of people >age65 living with SCD, our estimate suggests that there may be several thousand more people living with SCD than what is generally believed (100,000 per US CDC). Our estimates are partially validated by our finding that hospital claims data correlate strongly with our estimates of SCD prevalence at the state level. Although only a relatively small population of people living with SCD reside in rural counties, lower utilization of hospital services, as measured by hospital claims data, suggest that rural populations may have an unmet medical need that is particularly striking. Although working with claims data and disease estimates based on census data introduces significant limitations, it is feasible that this type of analysis could help to direct resources to areas with greatest unmet medical need.
Disclosures
Gehrie:Instrumentation Laboratories: Honoraria; Grifols: Consultancy; Cerus Corporation: Honoraria.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal